ISSUE1330
Once thought to be a beneficial response to critical illness, hyperglycemia is now recognized as independently associated with death and other adverse outcomes in various groups of critically ill patients. Whether normalization of blood glucose by insulin infusion is beneficial in such patients has been a subject of debate in the critical care community. Some new guidelines have been published.1
CLINICAL STUDIES — Among 1548 patients (about 60% post-cardiac surgery) in a surgical intensive care unit (SICU) randomized to receive intensive insulin therapy (IIT) to achieve a target glucose of 80-110 mg/dL (4.4-6.1 mmol/L) or to standard therapy with a conventional target of 180-200 mg/dL (10.0-11.1 mmol/L), in-ICU-mortality was 4.6% with IIT and 8.0% with the conventional target, a 42% decrease.2 A similar study in 1,200 subjects in a medical intensive care unit (MICU) showed no significant difference in mortality between patients on the intensive protocol compared to those receiving conventional glucose control (37.3% with IIT versus 40.0% in the control group).3 A combined analysis of these two studies found more hypoglycemic events in the IIT groups (11.3% vs. 1.8%), but with no serious consequences.4
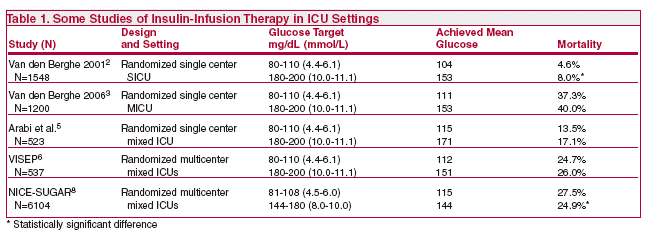
Another study (n=523) confirmed the increased incidence of hypoglycemia with IIT – severe hypoglycemia (glucose ≤40 mg/dL [≤2.2 mmol/L]) occurred in 28.6% of patients with IIT compared to 3.1% in conventionally treated patients – and found a 74% higher mortality (23.8% vs. 13.7%) in hypoglycemic patients, with no significant difference in mortality between IIT and conventionally treated patients.5
Among 537 patients in 18 ICUs with severe sepsis treated with IIT or conventionally, the rate of life-threatening hypoglycemia was significantly higher in the IIT group (5.3% versus 2.1%); there was no difference in mortality between the IIT and control groups, but the study was stopped early due to safety concerns.6
The Normoglycemia in Intensive Care Evaluation- Survival Using Glucose Algorithm Regulation (NICE-SUGAR) trial included 6104 medical and surgical patients in 42 hospitals. The target range glucose for the control group was 144-180 mg/dL and for the IIT group was 81-108 mg/dL. The results showed no significant difference in 28-day mortality (22.3% vs. 20.8%, P=0.17), but at 90 days the mortality rate was significantly higher in the IIT group (27.5% vs. 24.9%, P=0.02).7
A systematic review and meta-analysis of 26 randomized controlled studies of IIT in the ICU setting found no significant mortality benefit with use of IIT in the ICU (RR 0.93; CI 0.83-1.04).8
CONCLUSION — Clinical studies indicate that intensive insulin therapy with tight glycemic control (80-110 mg/dL [4.4-6.1 mmol/L]) is generally not beneficial for ICU patients, and may be harmful. Medical Letter consultants believe, however, that less intensive glucose control (140-180 mg/dL [7.8-10 mmol/L]) may prove to be beneficial. Whether some subgroups of ICU patients, such as diabetic patients post-cardiac surgery, would benefit from tighter control of blood glucose remains to be established.
1. ES Moghissi et al. American Association of Clinical Endocrinologists and American Diabetes Association consensus statement on inpatient glycemic control. Endoc Pract 2009; 15:353.
3. G Van den Berghe et al. Intensive insulin therapy in the medical ICU. N Engl J Med 2006; 354:449.
